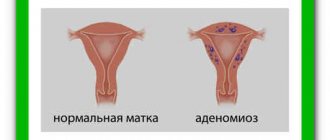
Proliferation of the glandular epithelium is an increase in the number of glandular cellular components that are localized in the cervical canal. This pathological condition is not an independent disease, but is considered rather a complex of cytological changes. Proliferation of glandular cells is not always a sign of a serious pathological process. In the vaginal part of the cervix there is a multilayered squamous epithelium, which performs a protective and regenerative function. The cervical canal contains columnar epithelial cells containing glands for the production of cervical mucus. Thus, signs of proliferation of the glandular epithelium are an increase in the number of glands, abnormal changes in their shape and structure.
Symptoms of pathological changes
An increase in the number of glandular epithelial cells of the cervix and their abnormally accelerated growth have different external manifestations. The variety of symptoms depends on the causes and nature of the pathology.
The reasons for increased proliferation of glandular epithelium are divided into pathological and non-pathological.
Among non-pathological causes, the most common is the use of oral hormonal contraceptives, which, with prolonged use, provokes the proliferation of the glandular epithelium. There is no need to worry too much about this, since areas with increased proliferation do not have a significant area.
It is especially important to pay attention to pathological causes. They may be:
- Pseudo-erosion of the cervix.
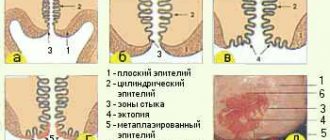
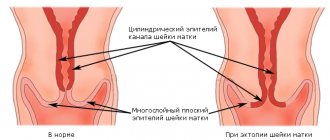
In this case, accelerated cell division of the glandular epithelium is observed in the area of the vaginal part, where stratified epithelium should be located in a healthy body. The disease can be diagnosed using a visual gynecological examination. The unhealthy area is clearly visible, as it has a different color from the normal (pink) mucous membrane - red (the epithelium, which is normally localized in the cervical cavity, is single-layered, and red vessels are visible through it). For a more accurate result, you can make a smear for cytological analysis, which will take into account the number of glandular components and their morphology.
Important! In case of pathological changes in the shape of cellular structures, it is necessary to immediately begin treatment aimed at eliminating the cause of the disease, otherwise the process may turn from benign to malignant.
- Infectious and inflammatory processes occurring in the vaginal cavity or in the cervical canal (colpitis and cervicitis).
As mentioned earlier, one of the functions of glandular structures is protective. In the presence of infection, the glandular epithelium “switches on” its characteristic protective mechanism: it increases secretion in order to replace the infected microflora and bring the infection out. Since these glandular structures are not adapted to a sharp and prolonged increase in functionality, they begin to change morphology, increasing in size, lengthening and twisting, which leads to a clear sign of the disease - compaction of glandular tissues.
The inflammatory process may also be accompanied by pain in the vagina and the appearance of discharge of a whitish hue and mucous consistency (leucorrhoea).
- Hormonal dysfunction is also a common cause.
The epithelium of the cervix is very susceptible to any fluctuations in hormonal levels; any hormonal disorder or disease of the endocrine system can provoke abnormal proliferation of this type of epithelium, it all depends on the individual characteristics of the patient.
In pregnant women, thickening of the epithelium in the cervical area is a consequence of natural hormonal imbalance, due to which the cervical epithelium is deficient in the influence of estrogen.
Symptoms in this case may include spotting between periods, dysfunctional uterine bleeding, and prolonged absence of menstruation (amenorrhea). The symptoms are also complemented by other external manifestations of hormonal imbalance.
- Trauma to the cervix can also trigger abnormal proliferation.
They can appear after a difficult birth, artificial termination of pregnancy, or medical procedures performed by an unqualified specialist. Due to injury, the integrity of the epithelium is disrupted; during the restoration of tissue structures, the glandular epithelium can grow and be localized below the cervical cavity.
Morphological classification
According to the generally accepted division of integumentary tissues, several types of epithelium are distinguished. Each of them has a set of individual characteristics, has a special structure and performs its own functions.
In morphological classification, it is customary to divide single-layer and multilayer epithelium. In the first case, it consists of cells of the same size and shape and is considered single-row. However, if its structure is formed by cells of different types. It is multi-row. in single-row epithelium :
- cubic;
- squamous;
- prismatic.
Multilayer epithelium is characterized by division into several types: squamous keratinizing, non-keratinizing and transitional. The first lines the surface of the skin on the human body and is called the epidermis. As they develop, the cells here transform into horny scales and remain on the surface. Gradually they peel off, giving way to younger cells.
The non-keratinizing epithelial layer is located on the cornea, oral mucosa, and in the esophagus. The structure is characterized by a multilayer arrangement and tubular shape of cells.
The deepest is the basal layer, consisting of basal cells. In this part, long cervical canals extend from the membrane and penetrate into the dermis. This ensures a strong connection with the underlying tissues. This is where stem cells and melanocytes are located, and melanin granules are found in large quantities.
Transitional stratified epithelium is so named because it can change its structure. It is integumentary in the following organs:
- renal pelvis;
- lining of the ureters;
- other urinary organs.
The main characteristic of these cells is their cubic shape and larger size. The condition changes due to a change in the volume of the membrane, but the connection of the cellular tubules with it remains.
Signs of the disease and basic information about the proliferation of glandular epithelium
Here is the basic information that is necessary to understand the nature and classification of this disease:
- Significant growth and compaction of glandular tissue in medicine is called hyperplasia;
- The treatment regimen is primarily determined by the localization of hyperplasia; highlight the proliferation of glandular epithelium on the surface of the vagina and in the cavity of the cervical canal;
- An important factor is also the degree of spread of the pathology: focal (spreads in nodular areas) or diffuse (uniform “offensive” spread);
- The stages of epithelial proliferation are an indicator of the progression of the pathological process (for example, moderate proliferation is characteristic of the formation of focal inflammation);
- Ectopias (or pseudo-erosions) are a sign of disorders of the glandular epithelium of the cervix, and glandular polyps (a consequence of focal hyperplasia) determine pathological changes in the epithelium in the cervical cavity.
If glandular proliferation of the cervical epithelium occurs without complications in the form of inflammatory processes, then the disease has no clinical manifestations and can only be detected in a laboratory.
Possible consequences of the disease
With properly prescribed treatment, the prognosis is favorable. Doctors resort to surgery only in extreme cases.
With timely prescribed therapy, all functions of the reproductive system organs are restored quite quickly and in full. A woman will have to come for routine examinations to a gynecologist every six months.
An unfavorable prognosis is possible with an advanced form of the disease or with incorrectly prescribed treatment. This condition leads to the development of infertility. This is due to the lack of ovulation and changes in the cellular structures of the epithelium.
In case of relapse of the disease, the doctor prescribes other drugs or those medications that have given a positive result, but in large dosages.
One of the most negative outcomes of the disease may be the transition of hyperplasia to a cancerous state. In this case, surgical intervention is most often resorted to. To exclude relapses of the pathology, a woman should be under constant monitoring by a gynecologist.
What are the forms of epithelial hyperplasia?
In histology, it is customary to distinguish 4 forms of epithelial hyperplasia:
- Simple.
The number of glandular epithelial cells increases in comparison with normal values. The walls of the uterus become denser, the tissues change morphology. The vessels on the inner surface of the uterus are normal. The cell nuclei do not undergo changes.
- Complex physiological.
Close confluent growth of epithelial cells. Abnormal cells are observed on the surface of the entire cervical cavity. The morphology of cells is pathologically modified. No deviation of the nuclei from the norm is observed.
- Moderate.
It is considered an independent disease. According to the description, it is transitional between malignant and benign forms of hyperplasia.
- Atypical complex (dysplasia).
The most dangerous form of hyperplasia. Cell atypicality is observed at the tissue and nuclear level, unlimited tissue growth, and no anatomical division into layers. With a high probability, the disease becomes malignant (cancer develops and progresses).
Diagnostics: identify pathology that occurs without external symptoms
As noted, hyperplasia (unaccompanied by an inflammatory process) does not have clinical symptoms, or has symptoms that are common for most gynecological diseases. Considering this, it is quite difficult to diagnose pathological changes in a timely manner.
Below is a standard set of gynecological diagnostic procedures designed to identify and classify this disease:
- Compiling an anamnesis by interviewing the patient in a similar manner;
- Visual gynecological examination on a chair;
- Colposcopy (colposcope is a magnifying device for optimizing the optical image of the cervix and vagina);
- Mucosal smear for microflora analysis;
- Biopsy and histological analysis (analysis of tissues with suspected pathological changes);
- Diagnosis of the pelvic organs using ultrasound;
- Study of hormonal levels;
- General blood analysis;
- General urine analysis;
- If a malignant change is suspected, the patient may be referred to a CT scan (or MSCT).
During a visual gynecological examination, “Nabothian cysts” can be detected (small semicircular formations formed from Nabothian glands filled with secretion). The proliferating glandular epithelium blocks the excretory ducts of these glands, thus clogging them and forming cysts. If Nabothian cysts were discovered during the examination, the disease is called glandular-cystic transformation.
It must be borne in mind that the proliferation of the glandular epithelium is often accompanied by the process of proliferation of the endometrium. Therefore, in addition to the endocervix (endocervix is the cervical canal that connects the vagina to the uterine cavity), the intrauterine mucosa must be carefully examined.
A mandatory diagnostic point should be a histological examination, the results of which are obtained by separate curettage of the surface of the uterus and the cervical cavity.
Hyperplasia during pregnancy
Pregnancy with hyperplasia is almost impossible. The egg does not fully mature, being in the pathological epithelium. Therefore, they do not extend beyond the ovaries. This becomes a common cause of hormonal imbalances in a woman’s body.
Even if the egg was able to fully mature and leave the ovary, pregnancy will not develop, since the embryo will be rejected by the endometrium. Hyperplasia during pregnancy can cause miscarriage. If the baby is nevertheless born, serious disturbances in the development of the child’s organs and systems may occur.
Possible treatments
Pathological proliferation of the glandular epithelium can only be effectively treated with complex therapy, which does not simply eliminate the consequence (hyperplasia), but targets the cause that provoked the disease.
If pathogens of infectious diseases are detected, it is recommended to carry out antibacterial therapy. An adequate treatment regimen is prescribed by the attending physician after identifying the causative agent of inflammation.
If you have hormonal imbalances, you should start taking hormonal medications as prescribed by your doctor.
As for the affected glandular epithelium itself, the only treatment option for this pathology today is destruction of the area of the mucosa with increased proliferation. This can be done using:
- Diathermocoagulation (a kind of “cauterization” of the mucous membrane using electric current);
- Laser destruction;
- Cryodestruction (freezing of the mucous membrane);
- Destruction using radio waves.
After such procedures, the cervical mucosa usually quickly regenerates and recovers without pathological deviations from the norm.
In advanced forms of cervical dysplasia (malignant processes), surgical intervention is required, which, in some cases, involves hysterectomy (amputation of the uterus).
Important! Considering the difficulty of identifying pathology by external symptoms, regular visits to a gynecologist for preventive consultation should be a necessary precaution.
If you liked this article, share it with your friends. After all, only timely detection of diseases and regular preventive measures can ensure a healthy and happy life.
Video: epithelial tissue. Glandular epithelia
Epithelial tissues. Glandular epithelia