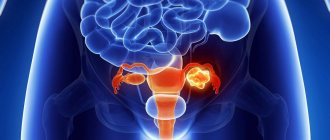
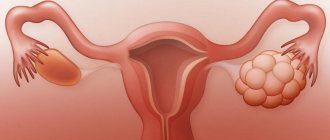
When gynecological problems arise, for example, ovarian cysts, which cannot be treated through drug treatment, one has to resort to surgical methods. Many women fear that this will negatively affect their reproductive function and are puzzled whether it is possible to become pregnant in this case. Depending on the type of cystic formations, the quality of the operation, and the absence of difficulties in the recovery period, pregnancy after removal of an ovarian cyst can be planned following the advice of doctors. This will give you a chance to carry and give birth to a healthy baby.
Causes
The formation of a cyst on the ovary can be caused by various factors.
- This also includes hormonal imbalances associated with taking contraceptives, hormonal drugs or an unhealthy lifestyle. Hormone-based contraceptives are not dangerous for women if they are prescribed by a doctor and are not a means of self-medication.
- Another reason is previous surgical interventions, possibly also to remove tumors. Relapses in this case also occur.
Other reasons include:
- promiscuous sex life,
- diseases of the endocrine system,
- There are chronic diseases of organ systems that interfere with normal hormonal levels.
Types of surgeries to remove ovarian cysts
If a woman is diagnosed with a cystic ovarian formation, she is prescribed a set of diagnostic procedures to determine the degree of threat to her health and reproductive function. The development of some types of cysts leads to disruption of ovarian function, negatively affects hormonal levels, and eggs lose their ability to mature normally. Large neoplasms can put pressure on neighboring organs; pedunculated cysts are dangerous due to the possibility of twisting of the base. After diagnosis, doctors determine treatment tactics and, if necessary, choose a surgical method.
- Surgery to remove an ovarian cyst
- Is it possible to get pregnant with an ovarian cyst?
Operations are carried out:
- using the traditional method of laparotomy, through an incision in the peritoneum;
- using a modern minimally invasive laparoscopic technique that allows manipulation (cauterization, excision) inside the abdominal cavity through several small punctures.
Surgical intervention techniques differ in the nature of the manipulations performed on the ovary. In simple cases, when the cyst cavity is not fused with the ovary, the cystic contents are sucked out, the cavity itself is cut off, suturing the ovarian tissue. In the presence of small multiple cysts (polycystic), electrocoagulation is performed. Sometimes it is necessary to excise part of the ovarian tissue along with the cyst.
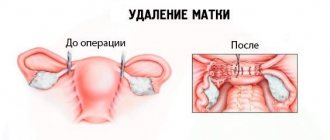
Operations are carried out in such a way as to preserve healthy ovarian tissue as much as possible and not disrupt their activity, so that reproductive function does not suffer in the future. In some cases, if a woman was inattentive to her sexual health, did not go to the antenatal clinic, or advanced the disease, which led to complications in the form of suppuration or tissue necrosis, forced removal of the cyst along with the ovary is required. After such an operation, the possibility of getting pregnant is significantly reduced, and even if you manage to conceive, pregnancy and childbirth can be quite difficult.
Effect on pregnancy
The formation of a cyst, which does not resolve with medication or with the onset of the next period, changes a lot in the functioning of the reproductive organs and hormonal levels. First of all, a follicular cyst significantly affects the level of hormones in the blood and when ovulation occurs. Sometimes it is the cyst that becomes the reason that ovulation does not occur, since the place of the follicle is taken by a neoplasm.
In addition, the tumor can put pressure on neighboring organs, interfering with their functioning. If there is a thin ligament between it and the ovary, torsion of the ovarian stalk may occur, and accordingly, there can be no talk of any ovulation.
Treatment
First of all, the nature of the neoplasm should be identified in order to understand whether pregnancy will occur after removal of the ovarian cyst. Some cysts go away on their own with the onset of a new cycle - this often happens with follicular cysts. Others actually require removal if after a new cycle they have not resolved, but continue to increase in size.
Treatment can be medicinal, involving the administration of drugs to resolve the cyst or hormonal drugs. Hormonal drugs are taken strictly after diagnostics and laboratory blood testing for the concentration of a particular hormone have been carried out.
Expected effects after tumor removal
After the operation, the woman’s condition improved:
- Hormonal levels are normalized and ovulation is restored,
- The pressure of the cyst on the pelvic organs is eliminated,
- Unpleasant symptoms go away: bleeding, pain in the lower abdomen, difficulty urinating and defecating,
- Risks to the fetus in the early stages of pregnancy disappear (tumors located near the uterus interfere with its growth and lead to spontaneous miscarriage).
The effect of the operation will be determined by the nature of the ovarian pathology. Restoration of hormonal levels is observed after removal of endometrioma and follicular cyst. These formations affect ovulation and inhibit oocyte maturation. Other cysts (dermoid, serous, paraovarian, luteal) do not interfere with the conception of a child, but can create mechanical obstacles to fetal growth. The greatest danger is caused by formations of large sizes - from 6-8 cm in diameter.
It is important to know
When planning pregnancy, it is recommended to remove an ovarian cyst that has reached a size of 3-4 cm, regardless of its type and the presence of symptoms.
Before planning a pregnancy, it is advisable to get rid of the cyst in order to avoid potential risks to the health of the woman and the unborn child.
Surgical removal
Surgical removal of the cyst is possible using the traditional surgical method with an incision, or laparoscopically using modern equipment and without large incisions. The second method is more preferable in modern medicine. This is due to the fact that it provides the woman with less inconvenience and causes less injury to the body.
In addition, the body directs all its forces to scarring the former ligament between the cyst and the ovary, and less energy to heal the wound. In the case of traditional removal, wound healing takes much longer.
The postoperative period lasts several days after laparoscopy, while after traditional surgery it may take a week or more. The most important thing is that after the cyst is removed, the patient’s body is thoroughly examined for possible complications.
Probability of pregnancy
The question of whether it is possible to get pregnant in this case worries many women who have undergone such an operation. If the necessary examinations were carried out during the postoperative period and no complications were identified, then pregnancy after a cyst is quite possible.
In principle, with the normal course of the operation and rapid recovery, the probability of becoming pregnant is equal to the probability of those women who have never had such diseases.
If complications are discovered, a rehabilitation period will be required to restore the reproductive function of the pelvic organs.
Possible complications
The most common complications include fallopian tube adhesions. Since the ovaries and fallopian tubes are quite closely connected and do not function fully without each other, the fallopian tube is quite dependent on the condition of the ovary.
If, for example, the cyst was located near the junction of the fallopian tube with the ovary, adhesions may form directly in this area. The adhesions block the lumen of the fallopian tube, as a result of which the egg cannot leave the ovary and remains in the tube.
This risks not only that ovulation will not occur, but also that fertilization will occur in the tube itself - it is called an ectopic pregnancy. This condition is dangerous for the life of the mother and the unborn child, and therefore is not considered normal.
Another common complication is infection. It will still not be possible to achieve sterility of the air in the operating room, because infections can somehow penetrate inside and inflame the mucous membranes.
To prevent such phenomena, immediately after the operation an antibiotic is prescribed, which prevents the development of infection, but is as gentle as possible on the intestinal microflora.
After two or three cycles, when it returns to normal and the ovary returns to normal, an absolutely normal course of pregnancy and fertilization is quite possible.
pregnancy after ovarian cyst removal
Hey everyone! I am glad to welcome you to my diary)) My name is Alina, and I am now 34 years old, my husband is 35)), my son is approaching his third year))
Here's my planning story)
I had quite a few operations: appendicitis in childhood, at the age of 24, removal of part of the thyroid gland, after which I took thyroxine for life, at the age of 26, rupture of a corpus luteum cyst with hemorrhage (lapara), resection of the right ovary, at the age of 28, removal of a dermoid cyst from the left ovary, after this lapara the ovary does not want to work and is small in size. My husband and I got married when I was 28 years old and started planning. After half a year of planning, hormonal imbalance, I went to the gynecologist, all the tests were good, only in that cycle there was a cyst, so increased estradiol and decreased progesterone, then I retested everything was normal. The gynecologist prescribes OK, Regulon, to normalize the cycle. Two months of use, pregnancy withdrawal, hCG = 79, a week later menstruation, apparently it was BCB, then tests, treatment for cytomegalovirus. Planning again, there is ovulation almost every month, if it doesn’t, a follicular cyst forms, I confirm ovulation with an ultrasound, usually on 13.14 DC. But there is no pregnancy, and now I meet in my clinic a new doctor who did an ultrasound for me, this is a hirudotherapist, she advises me to treat with leeches, I read reviews about leeches on the Internet, I start walking, first two months of adaptation to them, then vaginal placements. On leeches, my cycle became like an hour, almost every day (before that I wasn’t particularly lame either, but there were delays), and my periods also became more abundant and painless (after BCB they became scanty and very painful, I took painkillers). After half a year, I became pregnant, and I didn’t drink anything, I just had leeches, and it so happened that we only had PA that month at 12.13 DC. Everything was as usual, as before menstruation, I often went to the toilet (not a little), and the spot was brown, but the menses didn’t come, I took a test and there were two bright ones, the next day hCG = 1600, the next day 4200, the next day day 12000. Then I was in storage with a detachment and hematoma, and thank God the baby was saved. I gave birth by caesarean section, at 42 weeks, to our son))). The pregnancy was not very easy, the tummy often ached and became stiff, but the tone was never improved. Now we are planning again, but there are problems with hormones and ovulation. My story turned out so quickly and briefly))) I hope I write my story before my next pregnancy))
Polycystic
Typically, this disease is characterized by the presence of multiple cysts on the surface of the ovary. They are formed at the site of the follicles. It happens roughly as follows: during the first half of the cycle, several follicles mature - on average, 7. One of them is designed to become dominant and produce an egg for further fertilization.
Due to hormonal disorders, disruptions, and the same reasons that cause the formation of a regular cyst, the maturation of the dominant follicle does not occur.
The eggs begin to mature in all follicles simultaneously, but their maturation stops at a certain stage. The follicles fill with fluid, which is collectively called follicular polycystic disease. It may even be caused by heredity.
Possible problems after surgery
The possibility of conceiving a child is greatly influenced by complications that arise after surgery. If the rehabilitation period goes smoothly, problems usually do not arise, and the woman becomes pregnant safely within the next year.
Adhesive process
This term refers to the formation of adhesions between and within the pelvic organs. Possible consequences:
- Connective tissue cords form in the lumen of the fallopian tubes, preventing the advancement of the egg and meeting the sperm. These same adhesions become the cause of ectopic pregnancy, when the fertilized egg attaches to the wall of the fallopian tube,
- Adhesions that appear on the surface of the ovary interfere with the release of the egg and inhibit ovulation,
- The adhesive process in the uterine cavity prevents the attachment of the fertilized egg and contributes to miscarriage in the early stages.
The adhesive process, as a rule, prevents the conception and bearing of a child.
The likelihood of developing adhesions increases after abdominal surgery, and there are explanations for this:
- The surgeon's instruments and hands come into contact with the ovaries and other organs,
- During the operation, the pelvic organs come into contact with air and dry out,
- Significant incisions and stretching of tissue are formed when creating access to the ovaries,
- There is a high probability of infection of the surgical wound.
With minimally invasive laparoscopic surgery, the risk of unwanted effects on tissue is minimized. There is no contact with air or the surgeon's hands. The likelihood of developing an adhesive process is reduced. Laparoscopic surgery is recognized as the gold standard for ovarian cyst removal and is practiced in many clinics.
Laparoscopy is a minimally invasive method for treating ovarian cysts. After such an operation, a woman recovers faster.
Infectious complications
Risk factors:
- Failure to comply with the rules of asepsis and antisepsis during surgery,
- The presence of inflammatory processes in the pelvic organs,
- Immunodeficiency states.
Infectious lesions of the ovaries and fallopian tubes lead to the development of salpingoophoritis. The maturation of follicles is disrupted, and conceiving a child becomes impossible. Concomitant infection of the uterus leads to the development of endometritis. The fertilized egg does not find a place to attach, and a miscarriage occurs. But even with successful conception of a child, there remains a risk of infection of the fetus, the formation of severe defects and termination of pregnancy.
Decreased ovarian reserve
When exfoliating an ovarian cyst, the doctor tries not to touch healthy tissue, but this is not always possible. If the stroma of the organ was affected during the operation, the ovarian reserve decreases. The number of follicles decreases and the likelihood of conceiving a child decreases. The risk of infertility increases when surgery is performed on both ovaries.
Repeated operation
Repeated surgery is possible if complications develop:
- Bleeding. Occurs in the early postoperative period and is accompanied by a sharp deterioration in the woman’s condition,
Repeated surgery is performed if bleeding does not stop within several days after the intervention.
- Infection of the postoperative wound and suppuration of the sutures. Observed in the first days after surgery. Accompanied by increased pain and the appearance of purulent discharge from the wound.
After repeated surgery, the duration of the rehabilitation period increases, and the chances of conceiving a child decrease. If severe complications develop, removal of the appendages may be required.
For your information
Following the doctor's recommendations reduces the risk of complications after surgery and improves the prognosis of the disease.
Treatment
Its treatment can be complicated by the fact that the removal of such small cysts itself is not always justified. It may cause more damage to the ovary than it does good. Some neoplasms, both single and multiple, require removal along with the pipe if the neoplasm has affected it as well. And even in this case, there is hope for recovery and pregnancy.
Treatment is primarily prescribed medication. Since the most common cause is a lack of estrogen in the body, properly selected hormonal therapy can compensate for this deficiency and supply as much hormone as required into the blood. Then the ovaries begin to function and the egg matures.
Often this treatment is sufficient to restore ovarian function. But the only trouble awaiting women is the possibility that polycystic disease will return again.
Is it worth getting pregnant with a cyst?
Doctors recommend treating ovarian cysts first, and
Is pregnancy possible after surgery?
then plan for children.
But in some cases, the disease cannot be cured with medication and there is a need for surgical intervention.
In this case, most women think: maybe it’s better to give birth first?
This position of girls becomes understandable if we remember that after surgery on the ovaries there is a risk of infertility due to the possibility of obstruction of the fallopian tubes.
Doctors disagree on this issue.
In many cases, you can become pregnant during a cyst. Often women's lesions are small and do not cause them much discomfort. In this case, the expectant mother should constantly visit the gynecologist, monitor her health and get serious about treatment after childbirth.
Most likely, due to the presence of a cyst, the girl will need to lead a quiet, measured life, avoiding special stress and strain. There is a great chance that the cyst will resolve on its own during pregnancy. But this all concerns functional formations.
Things get more complicated if the cyst causes disturbances in the normal course of life processes in the body. It is quite dangerous if the cyst does not get smaller, and after testing, a high level of a substance present in the blood of patients with ovarian cancer is discovered. Large cysts are also considered dangerous. Sometimes it can be more than 9 cm.
By oncological standards, serous and mucious cysts are dangerous, which are important to remove before pregnancy. If they are left in the body for a long time, they can cause cancer.
Dermoid and endometrioid cysts are considered not dangerous for pregnancy, since they do not affect pregnancy and the development of tissue areas in the ovary in which egg maturation occurs.
You should be aware that there is a possibility that during pregnancy the cyst will rupture or the pedicle will twist. In such a situation, urgent surgical intervention will be required. There is no guarantee that after this the pregnancy will proceed smoothly and that the child will remain alive. But doctors will do everything possible to preserve the life and health of mother and child.
Read: Vomiting after menstruation: causes and treatment methods